The following blog post is written by a 2023 SAFE Project Intern. Though some sections have been lightly edited for clarity and anonymity, it is otherwise presented in their own words.
I became an EMT going into my first year of college with the intent of gaining clinical experience as an aspiring physician. For me, becoming a doctor was something that I always dreamed of as a kid, as I was interested in science and I liked the idea of helping people for a profession. As I grew older, my reasoning for wanting to become a physician became more nuanced after learning more about the US healthcare system and its deficiencies.
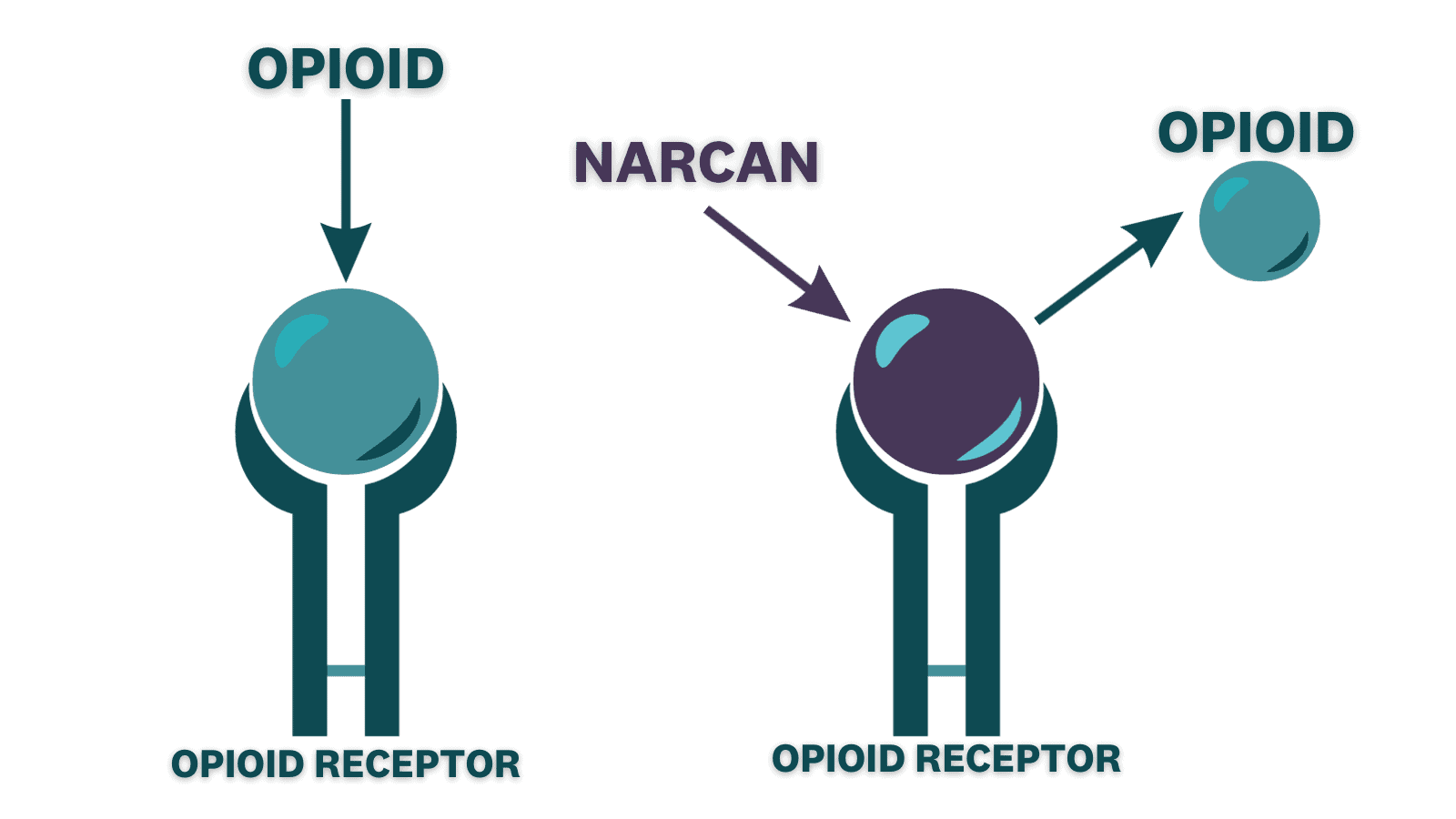
When I was learning about the different technical skills we were allowed to employ as an EMT, I learned about Narcan and became interested in how it works. It uses competitive inhibition to bind to the opioid receptor sites, thus removing the opioids that were already bound to them. Like with any other procedural training, we went over how to administer Narcan, but it did not feel real to me at the time.
It was not until about a month later that I was put in a hospital setting as a trainee as part of New Jersey state law for EMT training that I encountered someone who had overdosed on heroin. As a part of my training, my job was to take the vitals of the patients as they were transported to the hospital to ensure a continuum of care. An EMT had found her unconscious and had given her Narcan, but she was conscious by the time she reached the hospital. I remember that I was hesitant to take her vitals because she had track marks all over her arms, and I was afraid of treating someone addicted to drugs because of social training that warns against “these people.” Cautiously, I took her vitals and she remained lying in a stable condition on a hospital bed in the ER for about an hour before she started seizing. Her condition rapidly declined and doctors rushed to give her another dose of Narcan before ultimately having to perform CPR and defibrillating her. Unfortunately, this was not enough and she passed away.
This moment always lived with me because after her death I felt ashamed for the way I had regarded her. That moment was instrumental for me in defining the humanity of all people pushing past the social stigma against drug use. Additionally, I saw the importance of Narcan. Until that point, I thought Narcan was only used to stabilize a patient in the pre-hospital setting. I found out that it is a drug that saves lives and is even used by physicians.
Since that moment, although I have gone to calls where patients have overdosed, I have yet to administer Narcan personally, as conditions have been stable by the time I reached them. Nevertheless, I feel like I have become more comfortable with interacting with patients regardless of their backgrounds after that experience during my ongoing and future training.
