Reframing Relapse
Addiction is often defined or framed as a “chronic, relapsing disorder.” William White, a noted expert on addiction and recovery, points out that “…the lapse/relapse language within this phrase is historically rooted in morality and religion, not health and medicine, and comes with considerable historical baggage.”
Instead, when we accept that substance use or alcohol disorder is a disease, then we can understand that a relapse is the reoccurrence of symptoms associated with that disease. That allows us to stop stigmatizing someone’s actions as a moral failing. Just as a person with cancer or heart disease may have a reoccurrence of symptoms of their illness, our loved ones with substance or alcohol use disorders can also have a reoccurrence of symptoms – namely, a return to a previous or new substance or alcohol use.
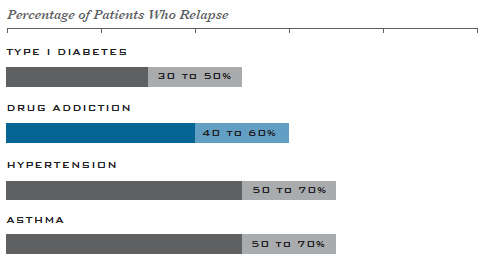
While many know that the first 90 days of sobriety (abstinence) are perilous, fewer people are aware that persons in long-term recovery can also experience a return, recurrence, or relapse. In fact, those relapse rates for drug or alcohol use disorders are similar to rates for other chronic medical illnesses. If people stop following their medical treatment plan for any disease, they are likely to have a reoccurrence.
Successful treatment for addiction typically requires continual evaluation and modification as appropriate, just like other chronic diseases. When there is a reoccurrence, that person needs to speak with their medical provider to resume treatment, modify it, or try another treatment.
There are factors believed to contribute to the reoccurrence of use, or relapse. One 2019 study highlighted areas that could indicate who is at increased risk:
- Younger patients were at increased risk of relapse.
- Having a co-occurring mental disorder was associated with elevated relapse risk.
- Risk of relapse/reoccurrence was related to characteristics of treatment sites.
There’s no one-size-fits-all risk –people in recovery may have their own unique indicators or warning signs. Recovery is a lifelong process, and relapse doesn’t mean someone failed. It can mean they may need some changes to their treatment plan and additional support. It can also be an opportunity for growth. “Reoccurrence isn’t a failure, it’s an opportunity to learn and grow,” reflects Brandee Izquierdo, a former Executive Director of SAFE who is in long-term recovery. “The knowledge that you’ve acquired in your journey isn’t lost. It’s a time to build in some extra tools, skills, and support”. Another way to frame the experience of reoccurrence of symptoms is “recovery disruption”. Leveraging this point of view recognizes that an individual, to Brandee’s point, hasn’t lost the knowledge and skills they have developed and honed in their recovery journey, but has been temporarily disrupted.
There is no shame in beginning again, for you get a chance to build bigger and better than before.
– Leon Brown
While a person’s recovery is their own responsibility, there may come a time when you see signs that your family member or child is having a recurrence of symptoms. Here’s how you can respond in a way that is helpful, but not damaging.
- Accept that people with diseases — such as cancer, diabetes, addiction, mental health issues — may have recurrences of that disease.
- Hopefully, you have tried to learn and understand everything you can about their specific challenge or disorder. This includes understanding their recovery plan if it has been shared with you.
- You may also have your own support group or system in place. If you don’t have one, check out our family support resources for connections to others who can provide help or resources.
- No matter how disheartened, angry, or worried you are, this is not an opportunity for you to shame them.
- Be supportive and empathetic, but don’t enable them. For instance, don’t cover for them if they miss classes, sports practice, or work.
- If you decide to talk to them, focus on the “I” statements and not focus on “you.” For example, “I am worried about” or “I noticed that…” is a better way to express concern than “What are you doing to yourself?” or “You need to try harder.”
- The most important role you can play is to be a source of support and encouragement. Your words and actions will show there is help, hope, and the opportunity to get back on track.
Learn More:
- NIH: The Science of Drug Use and Addiction: The Basics (Relapse)
- SAFE Project: The Science of Addiction
- Steven M. Melemis, Yale Journal of Biology & Medicine: Relapse Prevention and the Five Rules of Recovery
- Partnership to End Addiction: Understanding Risk for Relapse, Overdose, and What You Can Do
- William White Papers: Rethinking the Characterization of Addiction as a Relapsing Condition
